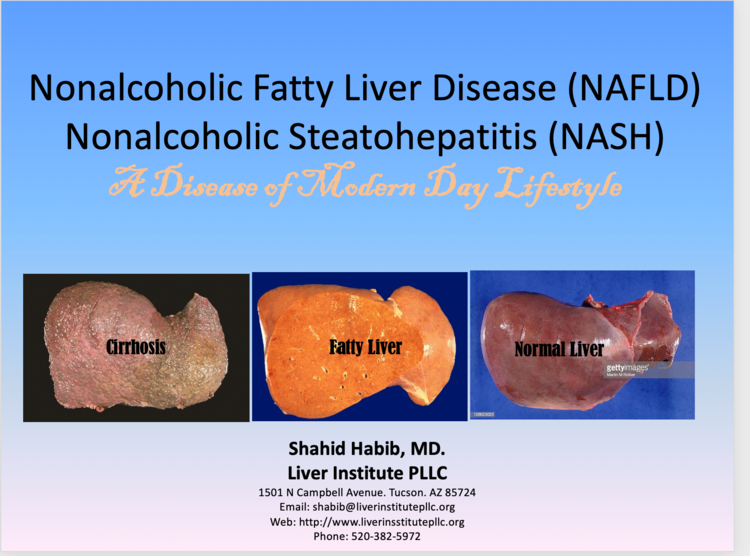
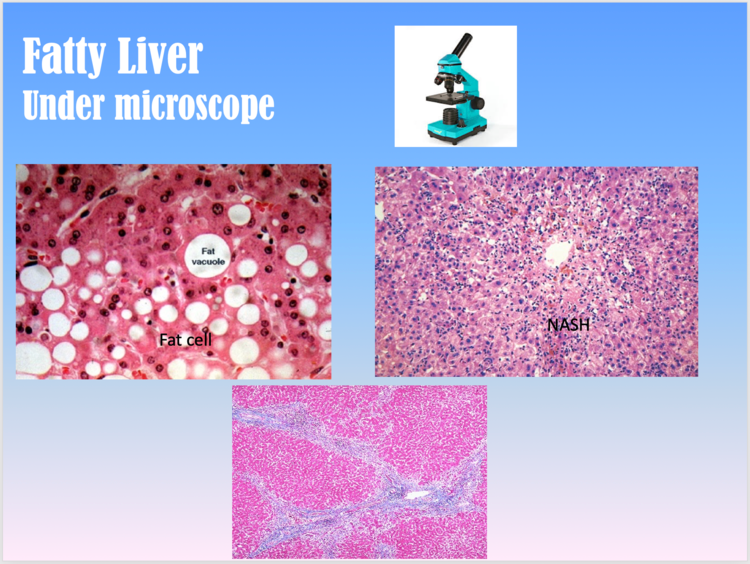
Fatty Liver
Metabolic syndrome (insulin resistance) NONALCOHOLIC FATTY LIVER DISEASE (NAFLD) NONALCOHOLIC STEATOHEPATITIS (NASH)
We offer more detailed and comprehensive treatment liver disease programs at The Liver Institute. We like to answer all your questions regarding liver disease and functions. Monitoring Dietary changes and activity levels is pivotal in the treatment of fatty liver disease. Our lifestyle and dietary appointments are tailored specifically according to your needs. We also offer options to participate in research studies related to the fatty liver for patients who meet the study requirements. Start your fatty liver treatment program, as recommended by Dr. Habib, by scheduling a consultation with our nurse practitioner for lifestyle and dietary appointments. Text us at 5203079094 to schedule.
A Disease of Modern-Day Lifestyle
UNDERSTANDING THE FATTY LIVER DISEASE AND CONSEQUENCES
What is a fatty liver?
Fatty liver is the accumulation of fats in the liver cells. The amount of fat in the liver depends on the balance between the processes of delivery, production, and removal. Accumulation of fat in liver happens as a result of impaired food processing in the liver. It means that more fat is being produced in the liver from ingested sugars and less fat is removal from the liver. Amount of ingested fat also play a role. In some patients, fatty liver may be accompanied by hepatic inflammation and liver cell death (steatohepatitis).
Does fatty liver affect your body functions?
Yes, fatty liver may affect your body functions. It is due to the lack of adequate delivery of nutrient to the rest of body resulting into fatigue and other body dysfunctions.
Is fatty liver a serious condition?
In proportion patients with fatty liver, fat accumulation into liver cell initiates the process of inflammation that leads to production of scar tissue ultimately reaching to the point of cirrhosis or nodular liver over 10-20 years. Subsequently, liver loses its functions and patient may need a liver transplantation to survive.
What is NASH?
Once, a patient exhibits all the features including fat, inflammation and scarring or fibrosis, the condition is called non-alcoholic steatohepatitis (NASH), which is sign of aggressive disease. Such patients usually develop cirrhosis and subsequent complications.
Who is diagnosed with NASH?
This that are diagnosed drink little to no alcohol, often have diabetes, obesity, and insulin resistance. It is often seen in people between 40-60 years old and the most common cause is insulin resistance and metabolic syndrome.
Why do people develop fatty liver?
Metabolic syndrome also known as Insulin Resistance (IR) caused by abnormal genes, over-eating, obesity, sedentary lifestyle. Medications can also lead to NASH/NAFLD.
What is insulin resistance or metabolic syndrome?
• It is malfunctioning of insulin hormone resulting into abnormal food processing in liver and transport of nutrients.
• Some may have more than normal amount of insulin hormone in their body.
How does your doctor diagnose metabolic syndrome or insulin resistance?
A. HOMA-IR score: It is calculated based upon blood tests: glucose and insulin level, normal value is less than 1.7, typically higher the value greater the severity of metabolic dysfunctions.
B. Metabolic syndrome is having 3 or more of the following traits:
1. Large waist: 35 inches for women and 40 inches for men
2. High triglyceride level: 150 mg/dL or higher
3. Reduced “good” or HDL cholesterol: less than 40 mg/dL in men and less than 50 mg/dL in women
4. Increased blood pressure: 130/85 mm Hg or higher
5. Elevated fasting blood sugar: 100 mg/dL or higher
Why does insulin resistance affect liver?
The liver is the organ where the ingested food is processed after being digested and absorbed from intestine. The liver also stores the processed nutrients and then deliver to the rest of the organs and tissues to develop and maintain their structure and functions.
How does insulin resistance affect liver? What are the associated symptoms?
Lack of adequate processing of ingested nutrients results into abnormal fat production, which is stored in the liver and abdomen as a free omental fat that causes big abdomen (belly), and if excessive, it overflows to other organs such as heart, great vessels (aorta). Fat accumulation and storage in the liver initiate events leading to inflammation and scarring (cirrhosis). Also, such abnormal fat accumulation causes abdominal pain and other gastrointestinal symptoms such as GERD and altered bowel habits.
Impaired food processing in the liver also results into inadequate production of required nutrients and impaired supply of nutrients to rest of the body. It results into relative malnutrition, which cause symptoms such as fatigue, lack of energy, and/or altered bowel habits. It may also affect sexual functions.
Why do providers care about NASH?
Approximately 10-30% of NAFLD patients will have their condition progress to NASH, and 20-30% of those patients will progress to cirrhosis. If this condition is not treated with intervention, there is poor long-term prognosis and patients are at a higher risk for developing hepatocellular carcinoma.
Is there other non-liver related condition associated with NASH that may increase the risk of death?
· Heart attacks
· Cancers, especially colon and esophageal
Can liver damage be reversed?
The liver is an organ that has the ability to regenerate. However, with the progression of liver disease, the regeneration is prevented in the presence of scar tissue in the liver. The scar tissue is present when there is ongoing damage that prevents regeneration.
TREATMENT OF FATTY LIVER DISEASE
a. Learning the Concept of Treatment
How do we treat fatty liver? Does lifestyle intervention help regenerate liver structure and improve functions?
Lifestyle intervention remains the backbone of all spectra of fatty liver disease treatment.
What is a lifestyle intervention?
Ø Energy Restriction
o Calorie Restriction (500-1,000 per day)
o 7-10% weight loss target
o Long-term maintenance approach
Ø Meal Timing
o Consume most calories during the day
o Light and Early dinner
Ø Healthy Fat Intake
o Low-to-moderate amount of vegetarian fat (polyunsaturated)
o Avoid saturated fat (animal fat sources including cheese)
Ø Low Glycemic Carbohydrates
o Avoid foods and drinks containing fructose
o Avoid white flour and corn products
Ø No Alcohol Intake
Ø Minimum 7 Hours of Sleep
Ø Coffee Consumption
o No liver-related limitations
Ø Physical Activity
o 10,000 steps per day
o 150-200 min/moderate intensity in 3-5 sessions
o Resistance training to promote musculoskeletal fitness and improve metabolic factors
What are the dietary goals?
· Sugars: 0 grams per day
· Protein: 1.2 grams per kg of body weight per day
· No saturated or trans fats
· 80% compliance
· 10% weight loss in the first year
b. Improved vigilance or self-education
How do we differentiate good carbohydrate from bad carbohydrate?
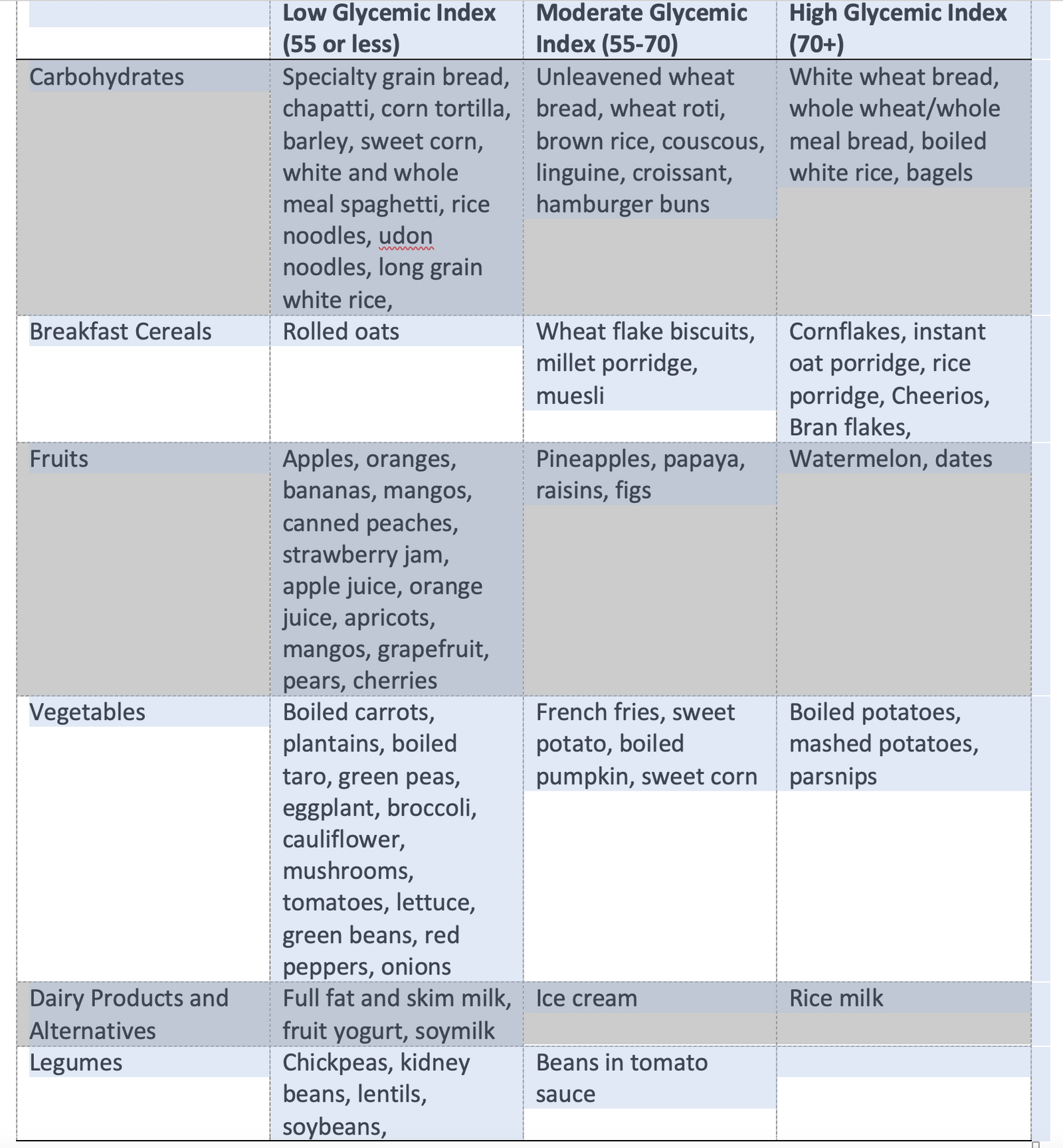
Glycemic index is the good measure to differentiate good from bad carbohydrate?
Glycemic Index of Foods:
· The glycemic index of foods measures how quickly or slowly the food can increase blood glucose levels. Low glycemic foods cause blood sugar levels to rise slowly and high glycemic foods cause blood sugar levels to spike rapidly.
What is the difference between saturated and unsaturated fats?
Saturated fats are solid at room temperature and are derived from animal sources such as red meat, whole milk, dairy foods, cheese, coconut oil, and are found in many processed foods. Saturated fats can increase total and LDL cholesterol which can lead to blockages in the arteries. Unsaturated fats are liquid at room temperature and are sourced from vegetable oils, nuts, seeds, and fish. Unlike saturated fats, unsaturated fats increase the levels of HDL cholesterol which removes other forms of cholesterol from the bloodstream and lowers the risk of heart disease.
Sources of Healthy Fats:
· Avocados
· Walnuts, cashews, almonds
· Olive oil
· Chia seeds
· Salmon
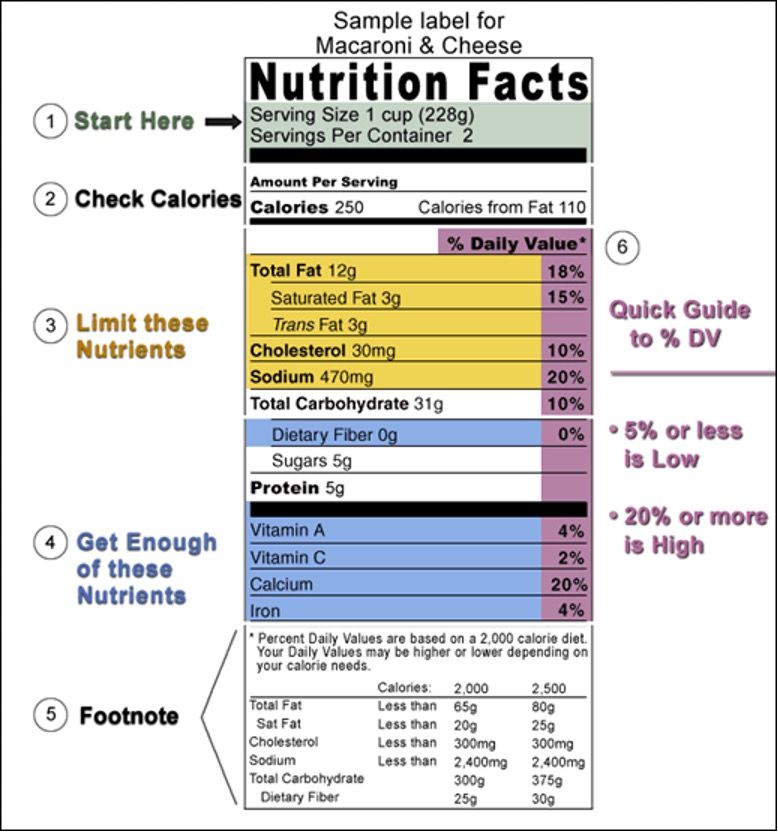
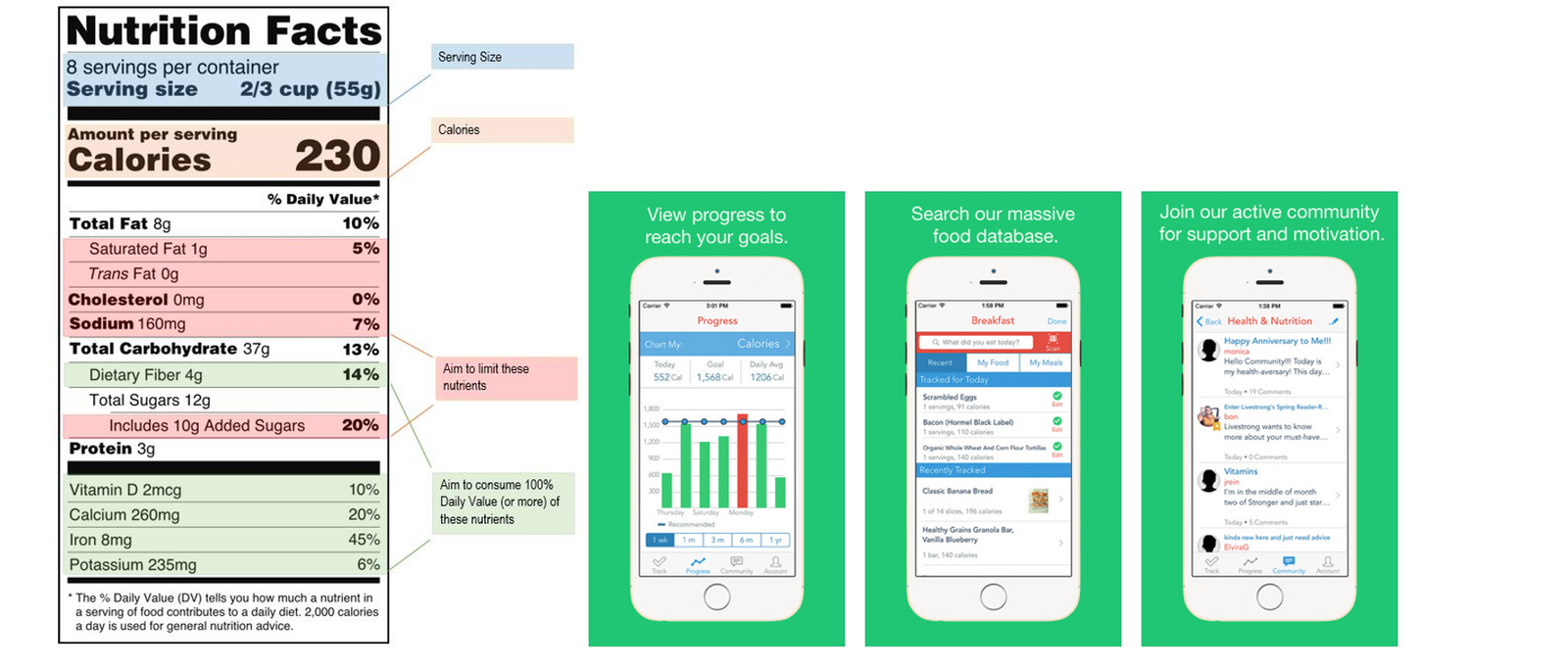
How to read nutrition labels:
Ø Make sure that if you are eating more that the serving size, to adjust the values accordingly.
o For example: If you at 2 cups of mac and cheese, that is double the serving size so you would also double the number of calories. For 2 cups of macaroni and cheese that would be 500 calories, 24g of total fat, 6g of saturated fat, 6g trans-fat, 60 mg of cholesterol, 940 mg of sodium, 62g of carbohydrates, 10g of sugar, and 10g of protein.
How to monitor daily caloric intake:
· Daily caloric intake can be tracked and measured using phone apps such as MyPlate or counting calories using nutrition labels.
o Calories can be tracked on MyPlate by scanning the barcodes of every food and beverage consumed and entering serving sizes for each meal and snack.
o Calories can also be tracked manually by reading nutrition labels and keeping track of serving sizes and calories.
How to limit caloric intake:
· Eat smaller portions
· Substitute sweetened beverages such as soda or juice with water or tea
· Limit the intake of saturated fat and processed foods
· Increase vegetable intake and lessen carbohydrates
How to monitor steps:
· Steps can be monitored using a pedometer or a phone app such as Google Fit (Android) or the Apple Health App.
Sedentary: < 5,000 steps per day
Low active: 5,000-7,499 steps per day
Somewhat active: 7,500-9,999 steps per day
Active: more than 10,000 steps per day
Highly active: 12,500 steps per day
Examples of moderate-intensity exercises:
· Brisk walking (2.5 mph or faster)
· Water aerobics
· Gardening
· Dancing
· Tennis Doubles
· Biking (<10mph)
Examples of resistance training:
· Free weights
· Medicine balls
· Weight machines
· Resistance bands

What is healthy plate look like?

What are the healthy drinks?

What are the recommended supplements?
Understanding some terminology:
Nonalcoholic Steatohepatitis (NASH): A condition that causes inflammation and accumulation of fat and fibrous tissue in the liver
Insulin resistance/metabolic syndrome: malfunctioning of the insulin hormone resulting into abnormal food processing in liver, some may have more than normal amounts of insulin in their body
è caused by abnormal genes, over-eating, obesity, sedentary lifestyle
Low calorie: 40 calories or less per serving
Low cholesterol: 20 mg or less and 2 g or less of saturated fat per serving
Reduced: At least 25% or less of the specified nutrient or calories than the usual product
Calorie free: less than five calories per serving
Fat free/sugar free: Less than 0.5 g of fat or sugar per serving
Low sodium: 140 mg or less of sodium per serving
Very low glycemic foods: foods that have a glycemic value index of up 40, hardly raise blood sugar at all
Low glycemic foods: foods that have a glycemic index value between 41-55, generally safe foods and does not spike blood sugar too quickly
Moderate glycemic foods: foods that have a glycemic index value between 55-70, best eaten with low or very low glycemic foods in order to help slow blood sugar release, no more than 2 servings per day
High glycemic foods: foods that have a glycemic index value above 70, should be eaten no more than one serving a few
Other important facts
- Older subjects of either sex have a lower energy expenditure and therefore lose weight more slowly than younger subjects.
- Food records are often inaccurate. Most normal-weight people under-report what they eat by 10 to 30 percent while overweight people under-report by 30 percent or more.
- Men lose more weight than women of similar height and weight when they comply with eating any given diet because men have more lean body mass and therefore higher energy expenditure.
Self-Monitoring record
• Get to know the food you are eating by reading nutrition fact labels
• Calorie counting
• Daily weight
• Waist measurement
• Track your activity with pedometer
• Make dairy of energy balance sheet
• Periodic assessment of achieving goals
• Follow up with provider (2-6 times per year) for NASH/NAFLD monitoring
Do you have question not answer yet?
Contact
Liver Institute PLLC