COLONOSCOPY
OVERVIEW
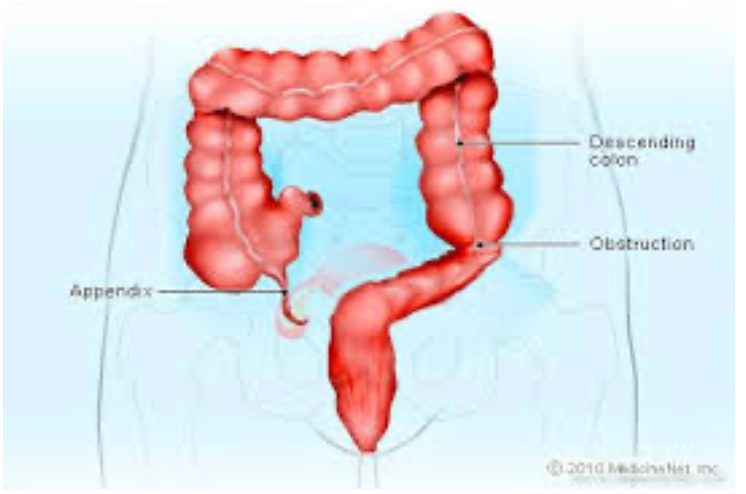
A colonoscopy is an exam of the lower part of the gastrointestinal tract, which is called the colon or large intestine (bowel). Colonoscopy is a safe procedure that provides information other tests may not be able to give. Patients who require colonoscopy often have questions and concerns about the procedure.
Colonoscopy is performed by inserting a device called a colonoscope into the anus and advancing through the entire colon. The procedure generally takes between 20 minutes and one hour.
REASONS FOR COLONOSCOPY
The most common reasons for colonoscopy are:
- To screen for colon polyps (growths of tissue in the colon) or colon cancer
- Rectal bleeding
- A change in bowel habits, like persistent diarrhea
- Iron deficiency anemia (a decrease in blood count due to loss of iron)A
- family history of colon cancer
- A personal history of colon polyps or colon cancer ●Chronic, unexplained abdominal or rectal pain
- An abnormal x-ray exam, like a barium enema or CT scan
GETTING READY FOR COLONOSCOPY
Preparation:
Before colonoscopy, your colon must be completely cleaned out so that the doctor can see any abnormal areas. This is vitally important to increase the chances that your doctor will identify abnormalities in your colon. If your colon is not completely cleaned out, the chances your doctor will miss abnormalities increases.
Detailed step by step instructions are listed below. Be sure to read these instructions as soon as you get them so you will know how to take the preparation and whether you need to make any changes to your medications or diet. If you have questions, call the doctor's office in advance.
Medicines:
You can take most prescription and nonprescription medicines right up to the day of the colonoscopy. Your doctor should tell you what medicines to stop. You should also tell the doctor if you are allergic to any medicines.
Some medicines increase the risk of heavy bleeding if you have a polyp removed during the colonoscopy. Ask your doctor how and when to stop these medicines, including warfarin, clopidogrel/Plavix, or any other anticoagulant (blood thinning) medicine. Do not stop these medications without first talking with your doctor.
Transportation home:
Most patients are given a sedative (a medicine to help you relax) during the colonoscopy, so you will need someone to take you home after your test. Your doctor may prefer that an anesthesiologist administer the sedative and monitor you during the colonoscopy. Although you will be awake by the time you go home, the sedative/anesthetic medicines cause changes in reflexes and judgment that can interfere with your ability to make decisions, like the effect of alcohol. You will not be able to drive home or go back to work after the examination if you received sedation for the procedure. You should be able to return to work the next day.
WHAT TO EXPECT
Before the test, a doctor will review the procedure with you, including possible complications, and ask you to sign a consent form.
An IV line will be inserted in your hand or arm. Your blood pressure, heart rate, and breathing will be monitored during the test.
THE COLONOSCOPY PROCEDURE
You will be given fluid and medicines through the IV line. With sedation/analgesia provided during the colonoscopy, many people sleep during the test, while others are very relaxed, comfortable, and generally not aware. Your doctor may request an anesthesiologist give you an anesthetic agent (for example, propofol), which is a stronger sedative and will put you to sleep while you are being closely monitored.
The colonoscope is a long black flexible tube, approximately the diameter of the index finger. The doctor will gently pump air or carbon dioxide and sterile water or saline through the scope into the colon to inflate it and allow the doctor to see the entire lining. You might feel bloating or gas cramps as the air opens the colon. Try not to be embarrassed about passing this gas (it is just air), and let your doctor know if you are uncomfortable. You may feel like you must go to the bathroom, which is a normal feeling during the procedure.
During the procedure, the doctor might take a biopsy (small pieces of tissue) or remove polyps. Polyps are growths of tissue that can range in size from the tip of a pen to several inches. Most polyps are benign (not cancerous). However, some polyps can become cancerous if allowed to grow for a long time. Having a polyp removed does not hurt.
RECOVERY FROM COLONOSCOPY
After the colonoscopy, you will be observed in a recovery area, usually for about 30 to 60 minutes until the effects of the sedative medication wear off. The most common complaint after colonoscopy is a feeling of bloating and gas cramps. You should pass gas and not feel embarrassed doing this either during or after the procedure. This will relieve your feelings of bloating and cramping. You may also feel groggy from the sedation medications. You should not return to work, drive, or drink alcohol that day. Most people can eat normally after the test. Ask your doctor when it is safe to restart aspirin and other blood-thinning medications.
COLONOSCOPY COMPLICATIONS
Colonoscopy is a safe procedure, and complications are rare but can occur:
●Bleeding can occur from biopsies or the removal of polyps, but it is usually minimal and can be controlled.
●The colonoscope can cause a tear or hole in the colon. This is a serious problem that sometimes requires surgery to repair, but it does not happen commonly.
●It is possible to have side effects from the sedative medicines like nausea or vomiting.
●Although colonoscopy is the best test to examine the colon, it is possible for even the most skilled doctors to miss or overlook an abnormal area in the colon.
You should call your doctor immediately if you have any of the following:
●Severe abdominal pain (not just gas cramps) ●A firm, bloated abdomen
●Vomiting
●Fever
●Rectal bleeding (greater than a couple of tablespoons [30 mL])
AFTER COLONOSCOPY
Although many people worry about being uncomfortable during a colonoscopy, most people tolerate it very well and feel fine afterward. It is normal to feel tired afterward. Plan to take it easy and relax the rest of the day.
Your doctor can describe the results of the colonoscopy as soon as it is over. If s/he took biopsies or removed polyps, you should call for results within one to two weeks if your doctor has not already contacted you.
PREPARATION FOR COLONOSCOPY
- PLEASE READ INSTRUCTIONS AT LEAST FIVE DAYS BEFORE YOUR PROCEDURE.
- IF YOU ARE TAKING BLOOD THINNING MEDICATIONS SUCH AS COUMADIN, LOVENOX, PLAVIX, ASPIRIN PRODUCTS OR FISH OIL CONSULT WITH YOUR PHYSICIAN FOR ADDITIONAL INSTRUCTIONS. ASPIRIN OR SIMILAR MEDICATIONS ARE USUALLY DISCONTINUED 7 (SEVEN) DAYS PRIOR TO THE PROCEDURE. Take your heart and blood pressure medication as usual the morning of your procedure.
- Purchase prep at any pharmacy (prescription was electronically sent to your pharmacy) and (2) tablets of Dulcolax laxative (no prescription needed). A commonly used preparation is a 4-liter (1 gallon) solution that is purchased at the pharmacy with a prescription. There are several low-volume (2- to 3-liter) preparations on the market as well. Refrigerating the solution can make it easier to drink, but do not put ice in the solution since it will melt and you will have to drink even more fluid. Drinking the solution through a straw, adding sugar-free powdered flavor packets (eg, Crystal Light), may also make it easier to drink. Do not follow instructions from pharmacy. This sheet is the only instruction you will need.
- 2 days before procedure: have ONLY clear liquids as much as you want. Solid food, milk, or milk products are NOT allowed. Acceptable clear liquids (a liquid you can hold up to the light and see through): Strained fruit juices without pulp, water, clear broth/bouillon, coffee/tea (without milk/creamer), Gatorade, soft drinks, Jell-O/Popsicles (NOTHING COLORED RED/PURPLE). You should also drink plenty of clear fluids on the day before the test. You can drink clear liquids up to 8 hours before your procedure.
-
Avoid drinking red liquids AND high fiber foods including seeds and nuts for the week before the procedure.
- The day before the procedure, at 4 P.M. take 2 (two) tablets of Dulcolax then drink the full amount of prescription prescribed and complete it by 8 P.M. To clean the colon, take the entire preparation the night before the test, or you may take it in two halves doses, finish first half dose in the evening and the second half dose taken six to eight hours prior to the colonoscopy. Taking the preparation in two "split" doses may help get the colon even cleaner. This prep causes multiple bowel movements. It may work within ten minutes or take as long as three hours. Remain within easy access of toilet facilities. You may continue to have clear liquids until 4 hours prior to your check in time. If your procedure is scheduled in the morning hours, then take the entire dose in the evening prior to the procedure.
- Diabetic Patients: NO diet sodas and juices. Drink regular sodas and juices during the preparation for this procedure. You will need the extra calories. (Diabetes Sheet will be given to you)
- After the prep, your stool should be clear to a yellow (Urine Color). If it is not, please call our office. If you do not follow these directions, your prep may not be adequate for us to complete your procedure, and you may need to reschedule.
- You must have someone drive you home: you will not be allowed to leave by yourself or drive for the remainder of the day.
- Included in this packet is an illustration and description of the colonoscopy and the technique that will be used during the procedure. Candice from Surgery scheduling will call you to schedule your procedure. If your insurance requires prior authorization, it could take up to 2 weeks for the approval to go through. Once it is approved, we will fax the order over to surgery for scheduling.
COLORECTAL CANCER SCREENING AND PREVENTION OVERVIEW
GOAL OF COLORECTAL CANCER SCREENING
Colorectal cancer is the term for cancer of the colon (large intestine) or rectum.
The primary goal of colorectal cancer screening is to prevent deaths from colorectal cancer. Screening tests can help identify cancers at an early and potentially curable stage. Screening can also prevent cancer by identifying and treating precancerous abnormal growths that can be removed before they become malignant.Adults should undergo colorectal cancer screening beginning at age 50 or earlier, depending upon their risk of developing colorectal cancer. Several tests are available, each of which has advantages and disadvantages. The optimal screening test depends upon your preferences and your risk of developing colorectal cancer.
WHY COLORECTAL CANCER SCREENING WORKS
Most colorectal cancers develop from precancerous polyps. Polyps are growths that form in the lining of the colon. They can be detected with an endoscopic procedure (colonoscopy or sigmoidoscopy) or CT colonography (see 'Colonoscopy' below and 'Sigmoidoscopy' below and 'CT colonography' below) and, to a lesser extent, by other tests such as the stool test for colorectal cancer.
The two most detected types of polyps are "adenomatous" and "hyperplastic." Adenomatous polyps (also called adenomas) can become cancerous over time; this progression takes at least 10 years in most people.
Colorectal cancer screening tests can detect polyps and cancers. If a polyp is found, it is removed to try to prevent it from becoming more serious. Regular screening for and removal of polyps reduces your risk of developing colorectal cancer (by up to 90 percent with colonoscopy). Similarly, if a cancer is found, it may be treated, hopefully at an earlier stage than it would have been found otherwise. Early detection of cancers that are already present in the colon increases the chance of successful treatment and decreases the chance of dying because of the cancer.
COLORECTAL CANCER RISK FACTORS
The risk of colorectal cancer increases as a person gets older, and most colorectal cancers occur in people older than 50 years of age. Therefore, experts recommend screening for people who are age 50 or older, even if the person does not have additional risk factors. (See 'Colorectal cancer screening plans' below.)
Some people have additional factors that increase their risk of colorectal cancer. Some of these impact recommendations for when to begin screening, while others do not.
Risk factors that may affect screening recommendations — Some conditions significantly increase a person's risk of colorectal cancer. Doctors often recommend that people with these conditions begin colorectal cancer screening earlier than people considered to be at average risk. (See 'Increased risk of colorectal cancer' below.)
Genetic familial syndromes: While uncommon, certain syndromes that are passed down in families can increase a person's risk of developing colorectal cancer. Having a first-degree relative (a parent, brother or sister, or child) with colorectal cancer increases your risk of developing colorectal cancer.
Personal or family history of colorectal cancer or polyps: People who have previously had colorectal cancer have an increased risk of developing a new colorectal cancer. People who have had adenomatous polyps before the age of 60 years are also at increased risk for developing colorectal cancer.
Inflammatory bowel disease: People with Crohn disease or ulcerative colitis have an increased risk of colorectal cancer. The amount of increased risk depends upon the amount of inflamed colon and the duration of disease; pancolitis (inflammation of the entire colon) and colitis of 10 years' duration or longer are associated with the greatest risk for colorectal cancer. (See "Patient education: Crohn disease (Beyond the Basics)" and "Patient education: Ulcerative colitis (Beyond the Basics)".)
Lifestyle risk factors — Certain lifestyle factors also seem to increase a person's risk of developing colorectal cancer. These include:
- A diet high in fat and red or processed meat and low in fiber
- A sedentary lifestyle
- Cigarette smoking
- Alcohol use
- Obesity
REDUCING THE RISK OF COLON CANCER:
Modifying these risk factors may help lower your risk of colorectal cancer, in addition to improving your overall health. However, the presence of these risk factors does not generally impact expert recommendations for when to begin colorectal cancer screening.
Factors that may decrease risk — As discussed above, improving your diet, getting more exercise, cutting back on alcohol, and quitting smoking (if you smoke) can all help lower your risk of developing colorectal cancer.
Using aspirin for prevention of cardiovascular disease may also decrease the risk of developing colorectal cancer. Because taking aspirin regularly comes with risks of its own, it's a good idea to talk with your health care provider before trying this.
Effectiveness of colonoscopy as a preventive measure – Colonoscopy is the most sensitive of the available tests; it detects most small polyps and almost all large polyps and cancers and substantially lower the risk of developing and dying from colorectal cancer.
Risks and disadvantages – The risks of colonoscopy, while small, are greater than those of other screening tests. Colonoscopy may lead to serious bleeding or a tear of the intestinal wall in some individuals (about 1 out of every 1000 people). Because the procedure usually requires sedation, you must be accompanied home after the procedure, and you should not return to work or other activities on the same day.
Contact us
If you want to cancel or reschedule your appointment, please call the Liver Institute as soon as possible.
